-
Pain Topics
- Ankylosing Spondylitis (0)
- Arthritis (5)
- Back Pain (35)
- Bulging Disc (3)
- Degenerative Disc Disease (2)
- Facet Joint Syndrome (1)
- Failed Back Surgery (1)
- Foraminal Stenosis (2)
- Herniated Disc (5)
- Kyphosis (1)
- Neck Pain (14)
- Osteoporosis (2)
- Paget's Disease (1)
- Pinched Nerve (3)
- Radiculopathy (1)
- Sciatica (5)
- Scoliosis (5)
- SI Joint Arthritis (1)
- spinal cord injury (4)
- Spinal Deformity (1)
- Spinal Fractures (3)
- Spinal Stenosis (2)
- Spinal Tumors (1)
- Spondylolisthesis (3)
- Spondylosis (2)
- Whiplash (2)
-
Treatment Topics
- ALIF (2)
- Artificial Disc Replacement (1)
- At Home Care (4)
- Chiropractic Care (3)
- Corpectomy (1)
- Diagnostic Procedures (2)
- Diet & Healthy Lifestyle (6)
- Everyday Ergonomics (2)
- Exercises & Stretches (4)
- Facet Joint Infection (1)
- Foraminotomy (2)
- Kyphoplasty (2)
- Laminectomy (2)
- Laminotomy (2)
- Massage Therapy (1)
- Microdisectomy (2)
- Minimally Invasive Spine Surgery (13)
- Nonoperative Solutions (7)
- Pain Management (6)
- Physical Therapy (2)
- PLIF (3)
- Revision Spine Surgery (2)
- Scoliosis Brace (2)
- Self-Care (7)
- Spinal Fusion (3)
- TLIF (3)
- XLIF Corpectomy (4)
-
Media & Interactive
What is Ankylosing Spondylitis or Bamboo Spine?
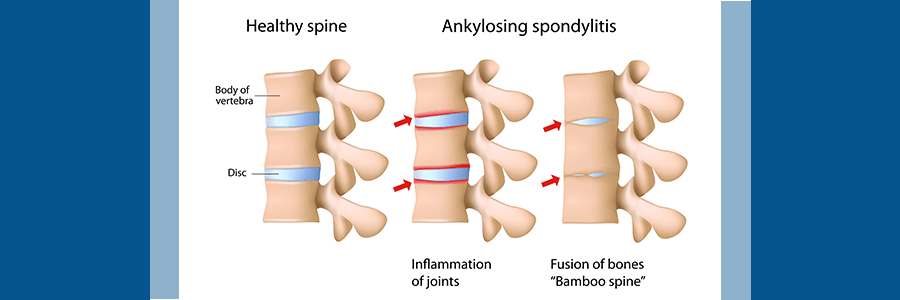
Ankylosing Spondylitis (AS) is a chronic inflammatory disease that affects multiple systems throughout the body. Usually, AS attacks the spine and sacroiliac joints, but it can also adversely affect other joints and organs as well. AS leads to spine-stiffening and inflammation in the joints. In rare cases, AS may even cause the spinal vertebrae to fuse. In fact, when vertebrae completely fuse together, this is known as ankylosis.
More accurately, AS causes the exterior fibers of the annulus fibrosus in our intervertebral discs to ossify, which leads to a spine that appears fused between each vertebra. Indeed, this is where the term “bamboo spine” comes from. The spine develops a bamboo-like appearance because of the joining of adjacent discs.
Causes of Ankylosing Spondylitis (AS)
The medical community widely believes that ankylosing spondylitis develops because of a genetic predisposition. The vast majority of AS patients are those who were born with the gene HLA-B27. In recent years, the medical community has developed blood tests to screen for this gene. In doing so, our understanding of the gene’s association with this condition has improved dramatically.
Of course, having this gene isn’t necessarily a sentence for developing AS. Studies show that additional factors—likely environmental—must be present in order for the disease to manifest. The reason for this belief is because of the way the numbers stack up. In the United States, 7% of people have the gene in question. That being said, only 1% of the population actually goes on to develop AS. So, while the gene is commonly found in patients who have the condition, it is certainly not the only factor at play.
Medical experts also suggest that genes ARTS1 and IL23R are responsible for the manifestation of AS. This belief exists mainly because these genes affect the way our body’s immune system works. The medical community generally accepts this as a notable risk factor for developing the disease.
It is still not well understood how the disease occurs and spreads to entirely different areas across the body. It is a very complicated ordeal, as every individual seems to have their own manifestation of the disease. Perhaps the disease came into play because of the body’s immune functions, or maybe it spawned from some sort of bacterial infection. The main point is that the disease is only understood in bits and pieces currently. The medical community is actively researching the disease to better understand how it works and how to best treat it.
Ankylosing Spondylitis (AS) Signs & Symptoms
The symptoms of AS are associated with the inflammation and arthritis in several different parts of the body, being: the spine, joints, and certain organs. With active inflammation, fatigue often accompanies the symptoms of AS. Spinal inflammation causes both stiffness and pain in the lumbar region, as well as the cervical area and upper buttocks. Of course, these symptoms may affect other parts of the spine as well. Usually, these symptoms are progressive, meaning that they only worsen with time and ultimately lead to a loss in overall range of motion. Additionally, the onset of these symptoms tends to be rapid and intense.
In severe cases involving the spine, a complete bony fusion between vertebrae may occur. When this happens, the pain disappears, but at the steep price of losing all spinal mobility. This new bamboo-like spine is quite brittle and vulnerable to fractures via trauma, such as with contact sports activities. Usually, the pain manifests suddenly when a spinal fracture such as this occurs.
Both spondylitis and ankylosis cause forward spinal curvature of the thoracic region. This limits the patient’s ability to breathe properly. Additionally, these problems affect where the ribs attach to the upper thoracic spine, which further decreases the patient’s lung capacity. As you can see, breathing becomes a major problem with AS.
Other areas affected by the condition are: the heart, eyes, and kidneys. Some patients with AS may develop iritis (inflammation of the iris). Iritis is easily identifiable by the redness and pain of the affected eye, which exacerbates when the patient is looking at bright lights. AS may also cause scarring in certain tissues of the heart, which in turn slows down the patient’s heart rate. Lastly, protein deposits (amyloid) in the kidneys from AS may lead to kidney failure in patients with the disease.

Ankylosing Spondylitis (AS) Diagnosis & Treatment
Usually, a doctor diagnoses AS through a physical exam—by asking the patient to bend into different orientations to examine the state of the spine’s motion range. After there is a rough idea of where to look, the doctor will then try to put pressure on specific areas of the pelvis and/or legs in order to find affected bodily regions.
Of course, doctors will also use imaging and lab tests as they see fit. For example, an MRI will help by showcasing all the details of the body’s bones and soft tissues. MRIs—although more expensive—will typically show signs of AS earlier than normal X-rays do.
There are also specific blood tests that a doctor performs to check for symptoms such as inflammation. However, this inflammation could theoretically come from anywhere—not just AS. It’s more likely that the patient’s blood will be tested for the HLA-B27 gene, even though most of these gene carriers don’t actually have AS.
Non-surgical Treatments for AS
There is a slew of treatments that doctors resort to when treating patients with AS. For one, doctors commonly give their patients NSAIDs (such as Naproxen) to help with inflammation. Additionally, these drugs may also help with the pain and stiffness that comes naturally with inflammation.
Sometimes, however, NSAIDs are not enough. In such cases, your doctor may try giving you a biologic medication, such as a TNF blocker. These medications target cell proteins in the body that lead to inflammation. TNF blockers also help with stiffness, pain, and sensitive joints. The doctor will administer this medication via an intravenous line underneath the skin.

Surgical Treatments for AS
The type of surgery that your spine surgeon considers for your case will depend on many variables. Such factors include your symptoms, the severity of the spinal abnormalities, your age, lifestyle, etc. It is not uncommon for a patient with AS to undergo more than one surgical procedure. Here are a few examples of the most common ones:
- Osteotomy:The surgeon cuts the bone to normalize angular deformities in the spine. After the doctor cuts and extracts the wedge, the bone ends are reunited so that they may heal together. Often times, your doctor will resort to rods, screws, and spinal fusion to help stabilize the spine during recovery.
- Spinal Instrumentation & Fusion: These procedures focus more on maintaining stability in the spine in addition to correcting the initial deformity. Fusion joins the bones together at the affected area so that bones may heal back together again. Rods and screws typically help with stability by holding the spine straight during this process.
- Laminectomy: Laminectomies are decompression procedures, which do exactly what they sound like they do. The performing doctor decompresses the spinal canal, which relieves nerves in the affected area thereby improving function.
Of course, these are just a few common examples. Make sure to communicate with your doctor to better understand your medical avenues.
Have you recently had a surgical procedure on your spine that didn’t quite work out? Still feeling stiff? Is it a pain just to stand upright? If so, you might want to give us a call at (855) 210-0899. It’s hard to live your life in chronic pain, so it never hurts to reach out to a team you can trust. Our spine surgeons will work tirelessly to ensure that you are put on a treatment plan that is tailor-made to suit your specific needs.
TAGS: Ankylosing Spondylitis
Explore New York City Spine

